
These days, gluten is a hot topic like never before. At a time when gluten-free products are becoming more and more trendy, we decided to separate the fact from fiction with the help of nutritionist Anthony Berthou.
So, what is gluten? Gluten is a protein found in certain grains which allows for seed germination. It is abundantly present in wheat but also to a lesser extent in other grains like oat, barley, and rye.
The word “gluten” comes from “glu” meaning adhesive, which helps us understand its role. Essentially, the gluten creates an elastic network in the dough when it is hydrated, allowing the dough to rise.
Only 1% of the population has a gluten problem: FALSE
Celiac disease is an autoimmune disease which affects about 1% of the French population (still, a large proportion of Celiac cases remain undiagnosed today – the statistic varies from 30% to 80% depending on the study). By contrast, we estimate that at least 5 to 10% of people are said to have a gluten hypersensitivity which can present as abdominal pain, fatigue, headaches, or even joint pain.
Gluten can cause problems in our bodies: TRUE
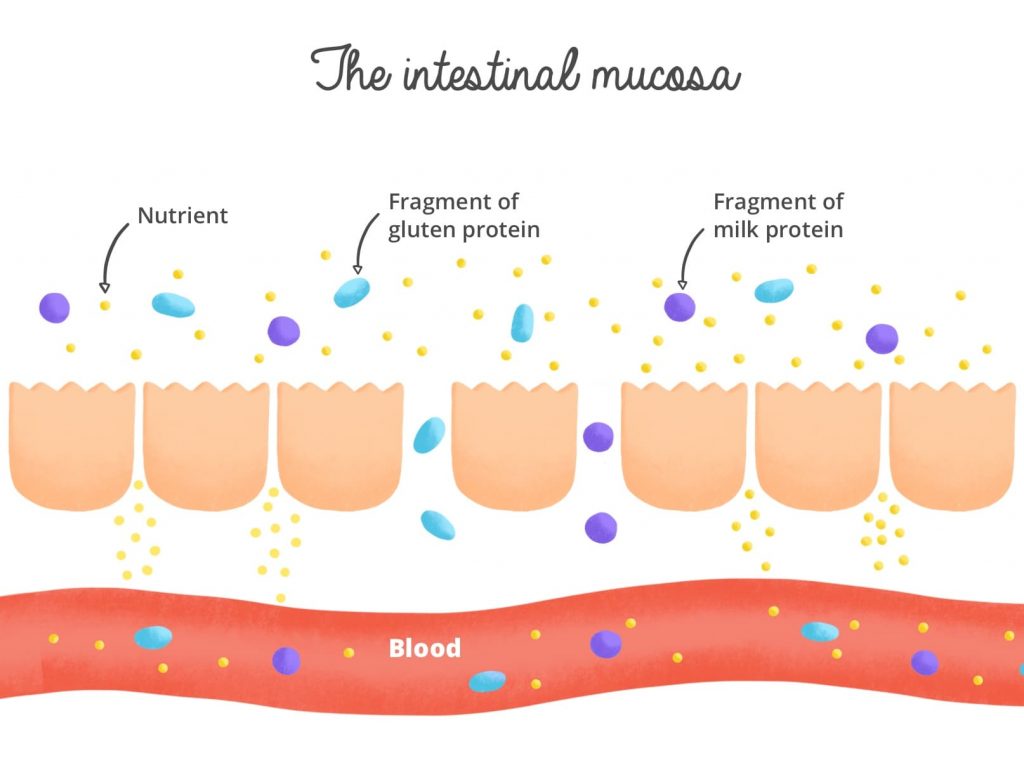
The small intestine’s job is to ensure the digestion of food and then the transformation of it into elements which can be absorbed by the body. The large intestine is made of a very thin lining: the intestinal mucosa. This intestinal mucosa serves an important protective function because it works as a barrier that prevents potentially toxic large molecules from moving into other parts of the body. It is also responsible for blocking the excessive passage of toxins, dangerous bacterias, or even viruses.
This mucosa is composed of very tightly-packed cells which make it impermeable. But different elements can attack the intestinal mucosa and intestinal microbiota, and as such, they can disrupt its function: taking antibiotics, consuming excessive amounts of protein, insufficient chewing, pesticides, sweeteners, high gluten consumption…
In these ways, they contribute to what we call intestinal permeability: they alter the junction between the mucous membrane cells, creating gaps between/within the cells. As a result, the intestinal barrier becomes more permeable and allows proteins to pass through that normally would have been blocked, like bacterial membrane extracts, gluten proteins, or even peptides which come from milk proteins! Imagine a colander whose holes are too big, so that it lets pieces of rice pass through; in the same way, the unwanted elements will also potentially pass through the intestinal wall and end up in the blood.
Our body will also try to defend itself against these elements that are not welcome in our blood, especially when the presence of these fragments in the blood is associated with a disruption in our microbiota (called dysbiosis).
This can lead to immune responses and inflammatory reactions, and it can contribute to the onset or perpetuation of functional disorders and food hypersensitivities. Particularly, we will mention indigestion, intestinal inflammation, migraines, increased risk for repeat infections, chronic inflammatory or autoimmune diseases according to genetic predisposition (eczema, asthma, multiple sclerosis, rheumatoid arthritis, Crohn’s disease, chronic ear infections and bronchitis, etc.).
What is the microbiota?
Our intestine is made up of about 100 trillion bacteria belonging to more than 1,000 different species. These bacteria make up what we call the microbiota (or gut flora).These good bacteria are essential to the healthy functioning of our bodies because they fight against bad bacteria and pathogens by helping to destroy them. They also serve us by defending against bacteria, viruses, and other parasites.
We know today that an unbalanced gut microbiota is linked to a wide range of illnesses like obesity, cardiovascular diseases, diabetes, certain cancers, mood disorders, neurodegenerative diseases, and auto-immune diseases such as multiple sclerosis.
But, don’t forget, it is not usually the act of eating one single piece of bread that is going to disrupt the body functions for the majority of people. Such an intense reaction is actually the result of a combination of factors, in particular:
- Genetic predisposition: certain individuals tolerate gluten more while others are more likely to experience symptomatic reactions.
- Disruption of the gut microbiota.
- The presence of other factors which disrupt intestinal permeability. Gluten is not the only substance which can disrupt this function, other elements contribute as well: excessive consumption of carbohydrates or proteins, insufficient chewing, repeated use of antibiotics, high consumption of cow’s milk, etc.
As such, if gluten consumption can lead to more intestinal permeability, the body’s response can vary according to the individual; a majority will never experience any side effects, while others could experience one of the reactions mentioned above. The part of the population vulnerable to a reaction still remains small (5 to 10% of individuals) and the scientific data is still too insufficient to establish a precise percentage of affected people.
Therefore, gluten can not trigger a disease on its own when there are neither an initial vulnerability nor other risk factors that could disrupt the role of the protective mucous layer. Such a type of reaction from the body is, above all, the result of a combination of factors.
Before, wheat caused fewer problems: TRUE
In order to increase output and feed the global population, modern wheat has been genetically modified through the crossing of many different varieties. The goal in all of this has been to shorten the grain for easier harvesting and to make it more resistant to disease. As a result of these crosses, wheat flour has become easier to handle and faster to knead, and its dough takes less time to rise.
This has contributed to increasing gluten “strength”, aka the dough’s capacity to stretch without breaking. This hybridization and selection of wheat varieties – which led to the production of stronger gluten – could explain some bodies’ heightened gluten sensitivities.
Einkorn wheat (also known as engrain) is an older variety of wheat compared to the modern wheat that we usually consume, and as a result, it triggers fewer inflammatory or immune responses.
Reducing gluten intake can help you feel better: TRUE
Unless you suffer from gluten hypersensitivity, there is no reason to eliminate gluten from your diet. On the other hand, reducing your gluten consumption can only improve your overall health, insofar as it helps to reduce the risks of mucous membrane damage. Provided, of course, that this choice is integrated into an overall balanced healthy diet.
Additionally, you should know that 10 to 40% of the population are intolerant to fructan. Fructans are a type of carbohydrate that we find in abundance in wheat and which will lead to digestive issues: diarrhea, bloating, gas, etc. If you regularly suffer from digestive issues, it is advised to eliminate all foods containing fructans and then to reintegrate them little by little, after allowing the entire gut ecosystem to rebalance itself. Besides gluten products, lots of vegetables contain fructans.
Eating gluten-free helps you lose weight: FALSE
Gluten is a protein: it therefore does not make you gain weight. A gluten-free diet can make you lose weight as a function of you eliminating bread, pasta, pizza, cookies or even pastries, assuming that you do not replace them with equally fatty or sugary gluten-free options.
Processed “gluten-free” food products are healthier: FALSE
When factory-made foods eliminate gluten in their products, manufacturers often add lots of additives to compensate for the loss of taste and texture. Additionally, eliminating gluten does not prevent a product from being too fatty, too sweet, or too salty. So, do not choose gluten-free options thinking that you are going to be eating healthier before looking closely at their nutrition facts.
A gluten-free diet can lead to deficiencies: FALSE
If eliminating or reducing one’s gluten intake means avoiding certain foods, it also allows us to vary our diet by integrating other foods like legumes (beans, lentils, chickpeas, etc.) or non-wheat grains (rice, buckwheat, millet, etc.).
Deficiencies can be observed only in the cases where gluten products are replaced only by nonnutritious industrial products, which is certainly not recommended.
- Alessio Fasano et al., Prevalence of Celiac Disease in At-Risk and Not-At-Risk Groups in the United States A Large Multicenter Study Original Investigation February 10, 2003 Arch Intern Med. 2003;163(3):286-292.
- Elma MJ Salentijn et al., Celiac disease T-cell epitopes from gamma-gliadins : immunoreactivity depends on the genome of origin, transcript frequency, and flanking protein variation BMC Genomics. 2012; 13: 277.
- Rubio-Tapia A et al, Increased prevalence and mortality in undiagnosed celiac disease. Gastroenterology. 2009 Jul;137(1):88-93.
- Paola Migliorini et al, Agronomic and quality characteristics of old, modern and mixture wheat varieties and landraces for organic bread chain in diverse environments of northern Italy European Journal of Agronomy Volume 79, September 2016.
- Alessio Fasano et al., Prevalence of Celiac Disease in At-Risk and Not-At-Risk Groups in the United States A Large Multicenter Study Original Investigation February 10, 2003 Arch Intern Med. 2003;163(3):286-292.
- Pulido O et al., Clinical features and symptom recovery on a gluten-free diet in Canadian adults with celiac disease. Can J Gastroenterol. 2013 Aug;27(8):449-53.
- Catassi C et al., Detection of Celiac disease in primary care: a multicenter case-finding study in North America. Am J Gastroenterol. 2007 Jul;102(7):1454-60.
- Rostom A et al., American Gastroenterological Association (AGA) Institute technical review on the diagnosis and management of celiac disease. Gastroenterology. 2006;131(6):1981–2002.
- Kelly CP et al., Advances in diagnosis and management of celiac disease. Gastroenterology. 2015;148(6):1175–86).
- Elli L et al., Diagnosis of gluten related disorders: Celiac disease, wheat allergy and non-celiac gluten sensitivity. World J Gastroenterol. 2015 Jun 21;21(23):7110-9.
- Suez J et al., Artificial sweeteners induce glucose intolerance by altering the gut microbiota. Nature. 2014 Oct 9;514(7521):181-6.
- Fasano. 2011 « Zonulin and Its Regulation of Intestinal Barrier Function: The Biological Door to Inflammation, Autoimmunity, and Cancer ». Physiological Reviews 151-175.
- Hollon et al. 2015. “Effect of gliadin on permeability of intestinal biopsy explants from celiac disease patients and patients with non-celiac gluten sensitivity”. Nutrients 7(3):1565-1577
- Melanie Uhde et al., Intestinal cell damage and systemic immune activation in individuals reporting sensitivity to wheat in the absence of coeliac disease Gut. 2016 Dec; 65(12): 1930–1937. Published online 2016 Jul 26.
- Aziz I et al., S. A UK Study Assessing the Population Prevalence of Self-Reported Gluten Sensitivity and Referral Characteristics to Secondary Care. Eur J Gastroenterol Hepatol 2014, 26 (1), 33–39.
- Biesiekierski J et al., Gluten Causes Gastrointestinal Symptoms in Subjects without Celiac Disease: A Double-Blind Randomized Placebo-Controlled Trial. Am. J. Gastroenterol. 2011, 106 (3), 508–514; quiz 515.
- Volta U et al., Serological Tests in Gluten Sensitivity (Nonceliac Gluten Intolerance). J. Clin. Gastroenterol. 2012, 46 (8), 680–685.
- Volta U et al., Study Group for Non-Celiac Gluten Sensitivity. An Italian Prospective Multicenter Survey on Patients Suspected of Having Non-Celiac Gluten Sensitivity. BMC Med 2014, 12, 85.
- Aziz, I.; Dwivedi, K.; Sanders, D. S. From Coeliac Disease to Noncoeliac Gluten Sensitivity; Should Everyone Be Gluten Free? Curr. Opin. Gastroenterol. 2016, 32 (2), 120–127.
- Moayyedi, P.; Simrén, M.; Bercik, P. Evidence-Based and Mechanistic Insights into Exclusion Diets for IBS. Nat Rev Gastroenterol Hepatol 2020.
- Roszkowska A et al., Non-Celiac Gluten Sensitivity: A Review. Medicina (Kaunas) 2019, 55 (6).
- Catassi, C et al., Non-Celiac Gluten Sensitivity: The New Frontier of Gluten Related Disorders. Nutrients 2013, 5 (10), 3839–3853. https://doi.org/10.3390/nu5103839.
- Volta U et al., Dietary Triggers in Irritable Bowel Syndrome: Is There a Role for Gluten? J Neurogastroenterol Motil 2016, 22 (4), 547–557.
- Catassi C et al., Diagnosis of Non-Celiac Gluten Sensitivity (NCGS): The Salerno Experts’ Criteria. Nutrients 2015, 7 (6), 4966–4977.
- Barbaro, M. R.; Cremon, C.; Stanghellini, V.; Barbara, G. Recent Advances in Understanding Non-Celiac Gluten Sensitivity. F1000Res 2018, 7.
- Molina-Infante, J.; Carroccio, A. Suspected Nonceliac Gluten Sensitivity Confirmed in Few Patients After Gluten Challenge in Double-Blind, Placebo-Controlled Trials. Clin. Gastroenterol. Hepatol. 2017, 15 (3), 339–348.
- Capannolo A et al., Non-Celiac Gluten Sensitivity among Patients Perceiving Gluten-Related Symptoms. Digestion 2015, 92 (1), 8–13.
- Elli L et al., Evidence for the Presence of Non-Celiac Gluten Sensitivity in Patients with Functional Gastrointestinal Symptoms: Results from a Multicenter Randomized Double-Blind Placebo-Controlled Gluten Challenge. Nutrients 2016, 8 (2), 84.





Such an informative article! But i do have a question: I play volleyball, and during the volleyball season, experience joint pain in my knees. Also, my joints are already weak, they have been my whole life, and I injured my elbow. It has healed, but now I need tape and a brace every time I play. Would going gluten free during my season help with these issues?
There are a lot of people who are sensitive to gluten that are not celiac sensitive. We have Hashimoto’s, Epstein Barr Virus and Lyme D. Over 500,000 people in the United States have Lyme. The biggest hurdle is recipes. When we were growing up hardly any of these auto immune things existed. Because, of the Floride and water and air issues, everything changes. Keto is a close runner up for a diet from gluten. Thank you for your app. I have used it and shared with a lot of people. Such a blessing.
Thee is one thing that is not mentioned, gluten is ONE of the hundreds of lectins produced by plants. All lectins are plant proteins which can bind to our cell receptors like viruses / bacteria and create havoc. Lectins are a problem not just gluten & bringing visibility to all of them would help a lot a people than just this gluten craze going on. The Plant Paradox of Steven Gundry has the whole scientific explanation. Did anyone read that book?
Very informative. Thank you. I have not come across an explanation of the complexity of gluten intolerance and it’s gut reactions. I have glu-intolerant friends.
Good summary.
Excellent Article! Will be forwarding.
I have an intolerance to wheat which causes a skin rash, dermatitis herpetiformis. I have only one of the two genes that cause celiac disease, and I can eat barley, rye and sourdough bread.
I learned a great deal from the article. Thank you for not being overly scientific though. Plain speak is much easier to understand. I am gluten sensitive and recently discovered that this was the main root in an inflammation problem I’ve had for almost 28 years. Doctors couldn’t figure it out and threw medication at it. I had an episode that landed me in the emergency room that caused me to re-evaluate my entire diet, which is when the gluten sensitivity was realized. You article confirmed something’s I suspected and taught me some new things. Thank you.
Very interesting article. Thank you! I am not gluten sensitive but try to avoid it by avoiding bread, pasta, etc… I am happy that you mentioned the Einkorn wheat as it is the flour I buy, knowing that it’s the best!
Why do you not mention the connection between wheat and roundup, which has contaminated the food supply?
Especially GMO’S !!
Missing from the article is that Wheat has been made easier to harvest by spraying Round UP on the crops to weaken the wheat and make it easier to harvest. I wonder how this plays into the conversation and how much of the problem is Gluten and how much is Round UP?
This is an excellent article! thank you.
Well written not overly medical or scientific, and easy to comprehend.
I’ve been avoiding gluten for several years and I feel much healthier.
Cheers,
Gary
Good article. As a Gluten Allergy hypersensitive I totally agree with all the True and False statement.